We are 1 st in Austin & Cedar Park, Texas
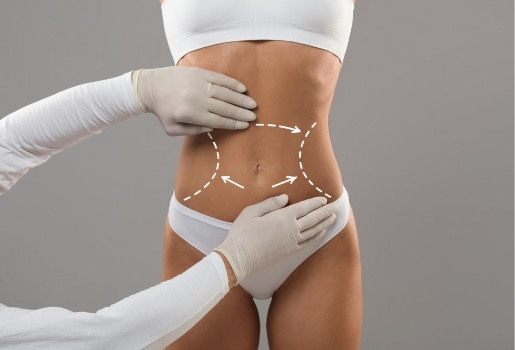
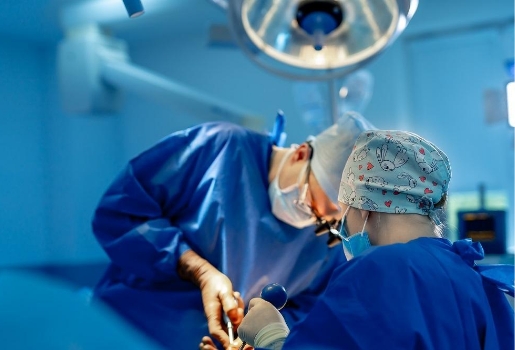
Read MoreLeading Weight Loss Surgery Experts in Austin and Cedar Park
Transformed over
Is Weight Loss Surgery right for you?
Take our 30 second assessment to find out and build your experience.
Take the Assessment
Leading Weight Loss Surgery Experts in Austin and Cedar Park
Transformed over
Is Weight Loss Surgery right for you?
Take our 30 second assessment to find out and build your experience.
Take the Assessment
Our Leading Bariatric surgeons in Austin and Cedar Park accept major insurance, self-pay, and offer financing options for affordable weight loss surgery. Self-pay patients can schedule surgery in about 2 weeks, and insurance patients once we receive the approval from insurance.
- 1st Single incision Lap band placement, umbilical approach with no visible scars in Texas was performed by Dr. Ganta
- 1st Gastric Sleeve procedure in Austin and Cedar Park was performed in 2006 in by Dr. Ganta
- 1st Duodenal switch procedure in Austin and Cedar Park was performed in 2006 by Dr. Ganta
Welcome to Nuself
Your All In One Destination for
* Bariatric Surgery * Medical Weight Loss
* Aesthetics * Advanced Davinci Robotic Surgery
Weight loss surgery is not the easy way out. It is a very effective and time tested medical treatment that changes your metabolism and helps you achieve your weight loss and health goals. In many cases it is the best medical treatment for conditions like diabetes, sleep apnea, high blood pressure, infertility, and many more.
Deciding upon surgery to lose weight, improve health, look better, become active and boost self-confidence is a big life-changing choice. Many think about it for years before deciding. The single most important decision you face now is choosing your team and partner in this life changing journey. You can place your absolute Trust and Confidence in Nuself to be your partner in this once in a lifetime journey towards a healthy and fulfilled life.
Nuself had been a trusted prover for over 5000 patients. We are pioneers in advanced techniques, highly skilled, experienced and also genuinely care about your overall success and wellbeing.Patients come from all over the US and internationally seeking care by Dr. Ganta. We believe in tailoring our solutions to match your goals, desires, and health concerns, creating a customized roadmap to your weight loss success.
All appointments are one-on-one Consultation with our surgeons. We do X-rays on same day of consultation for revision surgery patients so we can fully evaluate and create appropriate road map for success. We guide you through the process, answer every question, negotiate with your insurance and provide everything needed to make an informed decision regarding which procedure is best for you. We accept most insurance and self-pay patients can go to surgery in about 2 weeks.
At Nuself we don’t have just patients, we build relationships.
We serve Austin, Cedar Park and surrounding areas at one of our multiple locations.
Why NuSelf Bariatrics & Aesthetics?
Ready to redefine your journey to weight loss success? Trust NuSelf Bariatrics & Aesthetics to be your dedicated partner, offering not just treatments, but a personalized experience tailored just for you.

Dr. Ganta- The Pioneer and Expert in Single Incision Procedures in the Nation
Our legacy of innovation in bariatric surgery has made this transformative journey safer and more effective with proven long term results. Dr. Ganta’s pioneering single incision technique with no visible scar was showcased in his groundbreaking work in September 2008, when he performed the first trans-umbilical LAP-BAND® System weight loss surgery in Texas, leaving no visible scars. This Single Incision Laparoscopic Surgery (SILS) technique, with an incision of less than 1 inch artfully hidden in the navel, offers enhanced aesthetics and potentially quicker recovery with reduced discomfort. Dr. Ganta’s reputation as a leader in SILS has drawn experienced bariatric surgeons from across the nation to learn these innovative techniques.Dr. Ganta has achieved several “firsts” in Central Texas, including being the first to perform the Gastric Sleeve and the Duodenal Switch procedures.

“Your Trusted Experts with Proven Record of Success, Compassion, Dedication and Exceptional skill.”
When it comes to achieving your weight loss goals, Dr Ganta and Dr Juprasert don’t just provide treatments; they offer unwavering support and guidance throughout your entire journey. We use the most advanced technology, including daVinci Intuitive Robotic Systems for precision surgery. Our experts will be by your side, addressing every question and concern, ensuring you feel confident and informed.We recognize that each patient is on a personal mission, and our team is dedicated to crafting a treatment plan that aligns with your aspirations. Your goals become our goals. We treat patients like family. Many of our patients will attest, “You can’t go wrong with Dr. Ganta and Nuself.”

Our All-in-one destination to your Health, Weight loss and Aesthetic needs
At Nuself, we recognize that your path to vibrant health, weight loss, and personal transformation to looking and feeling your best is a journey, not just a destination. Dr. Ganta, Dr. Juprasert, and the team take a holistic approach to your health and weight loss journey and Aesthetic needs, providing comprehensive care before, during, and after your surgery under one umbrella. Our practice is your all-in-one destination for exceptional aftercare services, meticulously designed to nurture you through the physical and emotional dimensions of weight loss and your metamorphosis into a healthier and more radiant version of yourself for the rest of your life.

Surgical & Nonsurgical Options
Experience the latest in weight loss interventions with our advanced bariatric surgeries. Our state-of-the-art procedures are designed to cater to your unique needs, promising effective and lasting results.
Nuself offers a Full array of weight loss surgery procedures, including Complex revision surgeries, the LAP-BAND® System, Gastric Bypass, Gastric Sleeve, Sadi, Duodenal Switch, Gastric balloon, and Overstitch. Nuself specializes in Advanced Robotic Surgery techniques utilizing the latest daVinci Intuitive systems. Nuself is an expert in incomprehensive non-surgical and medical weight loss solutions, including the proven Skinny Shots / Semaglutide program. By combining surgical and non-surgical options, we can help you find a weight loss solution for your long term success.

Transformative Self-Pay Packages
Nuself Bariatrics offers some of the most value-driven, self-pay package prices in Texas. Our personalized care, vast experience, technical expertise, dedication to advanced bariatric surgery techniques, and all-in one destination packages present a remarkable value for our patients. We include 5 year routine follow-up and Aesthetic treatments as part of the package in addition to long term support. Our team is readily available to discuss our self-pay program options with you.

A Global Reach
Nuself Bariatrics served as a national training site, imparting advanced techniques for Single Incision Lap Band placement (the SILS band) to experienced bariatric surgeons. Additionally, patients from across the United States and around the world seek Dr. Ganta’s expertise, attracted by his accomplishments, dedication to innovation, outstanding success rates and compassionate care.
Insurance, Self Pay, and Financing Accepted

Insurance
Our office accepts most insurances to make bariatric surgery more affordable. We negotiate with insurance companies on your behalf to get surgeries approved if you have coverage.

Financing
Patients with out-of-pocket costs, from co-pays to the entire surgery cost, can split them into affordable monthly installments with financing.
Our Popular Services
Discover Our Leading Weight Loss and Cosmetic Services: Solutions that are at the heart of our clients’ achievements.
Gallery
“We don’t have just patients, We build relationships”
Watch Misty’s life-changing experience and see how Nuself can transform yours!
Here is the inspiring weight loss story of Raymond and Susan Cruz that changed their lives and can yours too!

Dr. Sashidhar Ganta
- Distinguished Board-Certified Surgeon
- Fellowship Trained at Yale University, an Ivy League Institution
- Nationally Renowned for Pioneering Single-Incision Lap band and Gastric Sleeve
- Mentor of Fellow Surgeons
- Topgun in Laparoscopic suturing
- Expert in Advanced Robotic Bariatric Surgery and Revisions
- A Proven Record of Over 5000 Successful Bariatric Procedures
Dr. Ganta, the visionary Founder of Nuself Bariatrics and Aesthetics, is a distinguished board-certified bariatric surgeon, renowned for his unparalleled expertise in Bariatric Surgery, serving the thriving community of Austin and Cedar Park, Texas. Driven by an unwavering commitment to transforming lives, he has amassed a remarkable record of over 5000 successful bariatric procedures, cementing his position as a true luminary in the field.
Dr. Ganta is not only a pioneer but also a master of innovation. He has trailblazed the path to excellence by pioneering and refining groundbreaking techniques such as the Single Incision Lap Band and Gastric Sleeve procedures. This pioneering spirit extends beyond his own practice as he generously shares his knowledge, having mentored and empowered numerous other surgeons to advance the field of bariatric surgery.
Dr. Ganta’s illustrious journey includes prestigious fellowships and a wealth of experience that have solidified his status as one of the foremost bariatric surgeons in the nation. At Nuself Bariatrics and Aesthetics, we take pride in offering a range of highly personalized weight loss solutions, including Primary and Advanced Revisions through the utilization of state-of-the-art Robotic Surgery techniques. Choose Dr. Ganta for an extraordinary bariatric journey toward a healthier, happier, and more vibrant life.















Dr. Jack Juprasert
- Board-Certified Surgeon
- Surgery Residency Training at Cornell University, New York, an Ivy League institution
- Bariatric Fellowship Training at the University of California, San Francisco
- Advanced Robotic Surgeon with Specialization in Antireflux and Bariatric Surgery
Dr. Juprasert, a board-certified general surgeon, renowned for his proficiency in the fields of bariatric surgery, hiatal hernia repair, anti-reflux procedures, and abdominal wall reconstruction/hernia repair. He exhibits a particular dedication to minimally invasive techniques, which not only enhance the aesthetic outcomes for his patients but also minimize postoperative discomfort. Dr. Juprasert’s surgical expertise spans across advanced laparoscopy, the da Vinci robotic platform, and interventional endoscopy, ensuring comprehensive and advanced care.
Born and raised in California, Dr. Juprasert’s journey in medicine began at the University of California, Santa Barbara, where he pursued a Bachelor’s of Science in Pharmacology. His fascination with the intricate workings of the human body and his desire to make a tangible impact on people’s lives motivated him to pursue a Medical Degree at Temple University School of Medicine in Philadelphia.




Our Blog

Understanding The Different Weight Loss Medications and How They Work
Are you struggling with weight loss and considering medical intervention? Weight loss medication may be the game changer you need.
Sep 1st, 2023 Read MoreExperience Matters
Nuself Bariatrics and Aesthetics is the trusted destination in Austin, Cedar park and central Texas for weight loss. Dr. Ganta is a highly sought after, pioneer bariatric surgeon with over 22 years of experience. He uses the SILS approach and the minimally invasive Da Vinci Xi® surgical system for bariatric surgery. Using the minimally invasive approaches patients can experience less pain and faster recovery.


This is life altering surgery! I wanted to know that person….look in the eye and trust that person. I met several surgeons and Dr. Ganta, and it was pretty much a no brainer at that point! I had 3 friends that had very successful surgery with Dr. Ganta and I wanted to be the 4th
Misty


I am just enjoying my best life and embracing my new body and just being confident! Working with Dr. Ganta was amazing! He cares about your well being before and after the surgery, even 3 and half years later he is involved which I like the most, and you don’t get that from a lot of doctors.
Tiereny


My Name is Meredith. One year and six months ago I had the sleeve gastrectomy procedure and since then I have lost 106 Lbs.
Meredith


When I started seeing Dr. Ganta I weighed 378 Lbs. As of today, I weigh 203 lbs. I’ve lost roughly 175-180 lbs.
Nate


Dr. Ganta is a very honest, straight-forward doctor. He lays out expectations, he won’t let you make excuses, and he’ll help you, that’s the most important thing.
Dana


I’m Dorothy, I had the gastric Sleeve done and I am currently down 96 lbs.
Dorothy
Our Patient Reviews
Discover heartfelt testimonials from our patients who have entrusted their health to our team – the true measure of our success.
Dr. Ganta is the absolute best Dr. I’ve ever had. When I was researching surgeons in my area I found him and refused to continue looking. It was either Dr.Ganta that would do my surgery or I just wasn’t going to have surgery at all. His education and experience are what drew me in. Then after meeting him I knew I had made the right decision. He’s very personable and is always willing to listen. And I’m that patient that goes in to every appointment with a list of 50 questions. When it came to my actual surgery I was extremely nervous but he assured me all would be well. I had the most amazing recovery with zero issues. Everyone is different but I didn’t even have pain immediately after. He really is the best and I love his staff as well. I’ve read some reviews that weren’t great about his staff but it seems that he finally has his long term crew and they are all great. Super friendly and always helpful when I need anything.
Autumn Chen

There are things I look for when finally seeking medical advice. 1- is knowledge 2- is comfort 3- how the office runs 4- care of the patient. Dr Ganta and his staff were the best at #4! Dr Ganta’s knowledge and calm behavior, with amazing listening skills made my experience the best! I hate hospitals and had extreme anxiety right before surgery, and Dr Ganta’s staff calmed my nerves and listened AND HEARD my fears. They never once made me feel less. They fixed it, and talked me through it. What Dr Ganta offers is weightloss surgery, but what you get as a patient, is full care every step of the way.
Marci Coursey

I knew I would have a great experience at NuSelf Bariatrics because I did thorough research on all of the bariatric surgeons and centers in Austin. Dr. Ganta and staff come highly recommended by so many individuals! Dr. Ganta’s staff were so personable and friendly. I felt noticed and valued! They each expressed their excitement for my journey and gave me their direct lines in case I needed anything or had questions. The office was clean and professional. COVID procedures were taken seriously. Ganta was composed, professional, thorough and amiable. He listened well, didn’t mince words, explained the procedure, risks and complications thoroughly and was very encouraging! Ill be having VSG on April 8th and I couldn’t feel more confident in Dr. Ganta and the wonderful team at NuSelf Bariatrics!
Andis Goble

Dr Ganta is consistently a top professional who is caring and addresses all my questions when I have a visit. He understands the needs of Bariatric patients in every way. I always look forward to my appointment because I know I will be treated well and leave with more understanding of my body and how it operates after a Bariatric procedure.
His office staff were very attentive and helpful with my vitamin questions.
Mary Ann Wallace

So so happy with decided to trust Dr.Ganta with my procedure. I made my initial appointment unsure of what procedure would be best for me. Dr. Ganta took his time and explained every procedure and what he thought the pros and cons would be for my situation. I’ve never had any doctor or surgeon care about me personally the way he did. My surgery was 5 days ago and I’m already up and about with minimal pain. I don’t think my pain tolerance changed overnight, so I’d like to think his expertise of preforming these procedures contributed to this. I had the SADI-DS for reference. All in all, nothing but positive for Dr.ganta and his entire staff. I’d recommend him to anyone who is even slightly considering bariatric surgery.
Carley Guidry

I had a gastric sleeve performed by Dr. Ganta on August 11, 2022. From my very first consult visit to my post-op visit today, Dr. Ganta and his staff have been incredibly attentive, compassionate, and competent. My surgery/recovery so far has been easy and without complication. I have had an amazing experience with this practice and Dr. Ganta is definitely a top expert in his field.
Abigail Murray

I am so grateful for the care and expertise provided from NuSelf Bariatrics and particularly Dr. Ganta. I recently required emergency surgery and am so thankful Dr. Ganta was the surgeon to do it. He checked on me daily during my post-operative stay and was readily available to the nursing staff to answer questions that came up. After I was discharged from the hospital I had a checkup with him and appreciated his questions as well as his answers to my own questions. I can’t recommend highly enough.
WE

Amazing experience. Have lost 27lbs in 4 weeks from Gastric Sleeve. Dr. Ganta is very analytical and cares about every single detail and concern, both before and after surgery. My blood sugar is now perfect, and had been Type II diabetic. My blood systolic pressure has dropped 30 points. I would recommend Dr. Ganta and his staff for anyone considering bariatric surgery. He is absolutely the most caring doc I have ever been to….
Dixie Barton

I had gastric sleeve done in March 2016, now I am almost 100 lbs down. Dr Ganta is amazing, he really wants his patients to succeed in their new bodies and life. Couldn’t ask for a better support system than with him and his staff. Everyone there are extremely polite and always ready to help you on your journey, you are not just a patient you become family. I drive almost an HR half to see him and very glad I do. If you are thinking of changing your life for the better, don’t go anywhere else than Dr Ganta and his team.
Dorothy Whiteman

I was sleeved by Dr. Ganta in January of this year. As a self pay patient I wanted to trust I was getting the best care for the money I was about to spend and I am 100% satisfied with Dr. Ganta. He has amazing bedside manner and everyone in his office is so kind and accommodating. Plus they don’t give you the surgery, then drop you on your own. The price I pad included a full year of monthly visits with Dr. Ganta and I feel fully supported. I HIGHLY recommend him if you are looking to have bariatric surgery.
Courtney McConnell

Dr. Ganta is THE BEST bariatric surgeon in Central Texas. He’s been my surgeon for over 15 years. I’ve had so much success with weight loss and it’s been all because of his expertise and staff. Everyone is helpful, patient, kind, and knowledgeable in the area of bariatrics. I would refer any of my family and friends to him without a doubt. Thank you, Dr. Ganta!
Tina Prentice

5 STARS. Dr. Ganta transforms lives with his professional expertise and supportive aftercare. The expansion of his cosmetic services are amazing and complement surgery. I just completed a new service BODYTITE to firm skin and eliminate fat cells. This procedure enhances stubborn body fat areas that hard to lose after surgery, as well as tightens and firms the extra skin. I highly recommend this procedure. It was in-office and painless and I am seeing amazing results already. His attention to detail and caring manner made the process successful. His office team is great and I felt cared for through the procedure. Thank you, Dr Ganta.
Collette Jamison

I am 100% satisfied with Dr. Ganta. He has amazing bedside manner and everyone in his office is so kind and accommodating… I HIGHLY recommend him.
COURTNEY M.

I am very thankful to Dr. Ganta and his staff for assisting me to become a better version of myself.
DANIELLE S.

If you are thinking about making Dr. Ganta your Dr… THINK No More… He is YOUR Guy… I LOVE YOU Dr. Ganta!!! Oh and the surgery was a success & I am a new person.
ADELA P.

Dr. Ganta is amazing, he really wants his patients to succeed in their new bodies and life. Couldn’t ask for a better support system than with him and his staff.
DOROTHY W.

I feel amazing and so much healthier. I appreciate the follow up appointments to help keep me on track and the support I have felt from everyone there.
ANDREA M.

Very professional and friendly
Dr.Juprasert is very professional friendly and easy to talk to 5 people found this helpful
Bella Ireland

Dr. Juprasert Appendectomy
Dr. Juprasert is a great communicator. We felt very informed about the process during my daughter’s appendicitis emergency. He checked in frequently in the hours following the surgery and was extremely patient and calm. Our emergency of course happened in the middle of the night but he was…
Stacy B

Fantastic surgeon! Great patient care!
I had to go in for emergency surgery, and Dr. Juprasert was very calm, explained the procedure well, and answered all my questions. He seems to really care for his patients! His patient care all around was excellent.
Sierra G

Asset to NuSelf Bariatrics
I had the pleasure of working with Dr. Juprasert after my gastric sleeve surgery. He takes his time and ensures that I understand all information discussed. Dr. Juprasert is never too busy to address my concerns, no matter how small. He even allows time during each visit to address all of my questions. He is definitely an asset to NuSelf Bariatrics. I’m beyond pleased with the care that he provides.
Joshua M

Great doc and on time
He is a great doctor and spent time with me to go over my history. On time so I didn’t have to wait
Jill Hudson

This office and Drs are great
It is about time that you can walk into a practice and discuss the difficulty of losing weight with a staff and Drs like Dr Juprasert and have them understand and support your journey to be healthy. This office wants you to be healthy. I tried shots and I did not tolerate them however I returned because I know the Drs and staff care. So today I start on a new plan and I am ready. Come to this practice it is great.
Alyce

Contact Us
We Look Forward to Meeting You
Our Locations
Austin
11851 Jollyville Road
Suite 104
Austin, TX 78759
South Austin
7201 Menchaca Rd
Ste B-1
South Austin, TX 78745
Cedar Park
500 W Whitestone Blvd
Suite 100A
Cedar Park, TX 78613
Instagram Feeds
Areas We Serve
Round Rock | Cedar Park | Pflugerville | Georgetown | San Marcos | Kyle | Leander | Buda | Taylor | Hutto | Elgin | Bastrop | Lockhart | Lakeway | Dripping Springs | Lago Vista | Manor | Wimberley | Liberty Hill | Smithville | Waco, TX | College Station, TX | Fredericksburg, TX | Temple, TX | Killeen, TX | Forthood, TX | Laredo, TX | Victoria, TX | New Braunfels, TX | Bryan, TX
© Copyrights 2024 NuSelf Bariatrics . All rights reserved.
 Book an Appointment
Book an Appointment